Executive Summary
- Maintaining between 40% and 60% RH in living and working spaces improves overall health and lowers
potential risk for transmission of viral diseases including influenza and COVID-19.
- Our bodies' natural defense mechanisms are impaired under dry indoor conditions.
- Humidification plays a vital role in indoor air quality.
Coronavirus, SARS-2-CoV, and COVID-19
In January 2020, a novel strain of Coronavirus, SARS-2-COV, emerged in mainland China,
and became pathogenic to humans.1 This virus is responsible for the current pandemic of COVID-19
(Coronavirus Disease). Symptoms of COVID-19 appear approximately 2-14 days from the point of infection.
The symptoms include fever, cough and body ache. A subset of infected individuals will experience more
dire symptoms including shortness of breath, persistent pain and pressure in the chest, which can lead
to pneumonia. These individuals should seek emergency medical care. Approximately 20% of total cases
require hospitalization. About half of hospital admissions are older adults (ages 65 and over),
an age group that faces the most serious complications of the disease.2
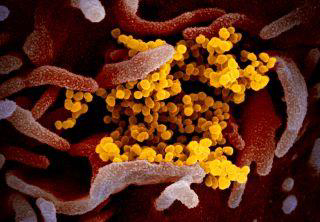
Figure 1: Scanning electron microscope image shows SARS-CoV-2 (yellow)
among human cells (pink). This virus was isolated from a patient in the U.S.
(Color has been added to the image to better show the virus and its environment.)
(Image: © NIAID-RML)
Humidification, Human Health, and Viral Infection
In cold climates where buildings and homes are heated during winter months,
relative humidity can fall below values ideal for human health (i.e. <30%).
This can cause dry skin3, irritated eyes4, and a persistent cough5.
Humidifiers are an ideal solution for making dry indoor air more comfortable.
Simple plug-in countertop humidifiers are popular in homes for temporary use when a resident is
suffering upper respiratory illness. Whole-home evaporative pad style humidifiers are often installed
in the supply-air duct near the furnace. These work well with heating systems that have high plenum
temperatures (>120°F). More and more homes are being heated by “heat pumps” which have low plenum
temperatures (<80°F), where pad style humidifiers are ineffective and electric steam (isothermal)
humidifiers are recommended.
In commercial spaces, isothermal humidifiers have become more prevalent in the
last 40 years, especially in healthcare facilities. This, in part, is due to ASHRAE guidelines6.
By raising relative humidity in indoor environments, humidifiers can improve
general health and well-being7-8. In addition, a variety of studies have shown the incidence and
the severity of viral diseases, such as those caused by coronavirus and influenza, are lower when
relative humidity is between 30% and 60%9-10.
People contract viruses (such as influenza or coronaviruses) when touching
surfaces or through contact with air contaminated with droplets of virus (e.g. from a cough or sneeze).
The viruses generally enter the body through the eyes, mouth, or airways.
Experiments have shown coronaviruses to survive for up to five days on stainless steel,
other metals, glass, paper, and Teflon11. They can remain active on some plastics for up to 9 days.
While we have limited understanding of SARS-2-COV, other coronaviruses and influenza viruses are
least infectious when RH is maintained near 50%12.
Once airborne, temperature and relative humidity influence the viability of
viruses by affecting the properties of the viral surface proteins and lipid membrane.
Results from experiments where viruses were nebulized into various indoor environments show the highest
stabilities at low (e.g. <40%) and high (>80%) relative humidity. These studies show the virus remains
infectious longer at low RH conditions typical of non-humidified spaces in winter13. Thus, humidifying
spaces may reduce transmission of influenza and coronaviruses.
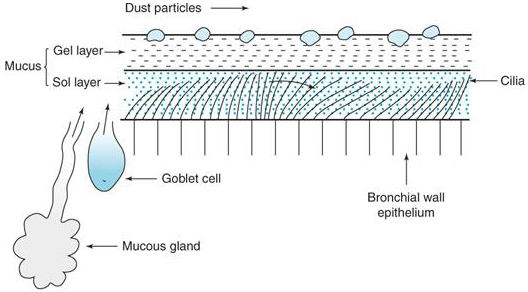
Figure 2: The MCC and underlying epithelium.
Damage to the MCC from dry air can increase risk of viral infection.
Both mucous glands and goblet cells contribute mucuous to the MCC
(Levitzky, MG; Pulmonary Physiology. Eighth Edition.
We are most commonly exposed to viruses through our respiratory
tracts. Mucus lines our upper airways and acts as the first intrinsic barrier against viral
infection. Mucus is over 90% water, thus it is important for our bodies to maintain hydration.
The inhalation of cold air, which is always dry due to the limited water vapor capacity,
can cause impairment of our mucocillary clearance (MCC, part of the self-clearing mechanism of
the airways in the respiratory system, Figure 2). When we warm cold environments without adding
humidity, it has the same effect. The MCC acts as a key mechanism for eliminating inhaled pathogens,
microbes and irritants from the respiratory epithelial surface. An impaired MCC will leave an
individual more susceptible to risk of viral infection.
Dry air can also damage the respiratory epithelial surface,
which is the second line of defense against viral infection. The continued inhalation of dry air
can cause epithelial cell loss, and the inhibition of cellular repair. Overall, the impact dry
air has on the integrity of our respiratory surfaces is thought to influence the prevalence of
respiratory viral infections during winter months14-15.
The impact of humidity on increased infection rates has been borne
out in empirical and population studies. Virus transmission between guinea pigs has shown to be
most efficient under low relative humidity16, similarly, low outdoor relative humidity was found to
contribute to the severity of MERS-CoV (Middle East Respiratory Syndrome) outbreaks17. These studies
concluded that in cold and dry climates, dry indoor conditions promoted transmission from aerosolized
viruses entering the respiratory tract, while in warmer more tropical environments contact transmission
was more prevalent.
In fact, recent building guidelines have outlined the critical need
for humidification to help optimize indoor air quality for human health18.
In summary, these points emphasize the positive role humidification
plays in offices and health care facilities on par with frequent cleaning of surfaces and handwashing.
For Neptronic Humidification Solutions visit our page or download PDF file.
References
- Andersen, K. G., Rambaut, A., Lipkin, W. I., Holmes, E. C., & Garry, R. F. (2020).
The proximal origin of SARS-CoV-2. Nature medicine, 26(4), 450-452. DOI: 10.1038/s41591-020-0820-9
- Rothan, H. A., & Byrareddy, S. N. (2020). The epidemiology and pathogenesis of coronavirus
disease (COVID-19) outbreak. Journal of autoimmunity, 102433. DOI: 10.1016/j.jaut.2020.102433
- Sato, M., Fukayo, S., & Yano, E. (2003). Adverse environmental health effects of ultra-low
relative humidity indoor air. Journal of occupational health, 45(2), 133-136. DOI: 10.1539/joh.45.133
- McIntyre, D. A., & Griffiths, I. D. (1975). Subjective responses to atmospheric humidity.
Environmental research, 9(1), 66-75. DOI: 10.1016/0013-9351(75)90050-X
- Strauss, R. H., McFadden, E. R., Ingram, R. H., Deal, E. C., & Jaeger, J. J. (1978).
Influence of heat and humidity on the airway obstruction induced by exercise in asthma.
The Journal of clinical investigation, 61(2), 433-440. DOI: 10.1172/JCI108954
- Paul Ninomura, P. E., & Richard Hermans, P. E. (2008). Ventilation standard for health
care facilities. ASHRAE Journal, 50(10), 52-57.
- Nordström, K., Norbäck, D., & Akselsson, R. (1994). Effect of air humidification on the
sick building syndrome and perceived indoor air quality in hospitals: a four month longitudinal study.
Occupational and environmental medicine, 51(10), 683-688. DOI: /10.1136/oem.51.10.683
- Reinikainen, L. M., Jaakkola, J. J., & Heinonen, O. P. (1991). The effect of air
humidification on different symptoms in office workers—An epidemiologic study. Environment International,
17(4), 243-250. DOI: 10.1016/0160-4120(91)90009-F
- Myatt, T. A., Kaufman, M. H., Allen, J. G., MacIntosh, D. L., Fabian, M. P., & McDevitt,
J. J. (2010). Modeling the airborne survival of influenza virus in a residential setting: the impacts of
home humidification. Environmental Health, 9(1), 55. DOI: 10.1186/1476-069X-9-55
- Noti, J. D., Blachere, F. M., McMillen, C. M., Lindsley, W. G., Kashon, M. L.,
Slaughter, D. R., & Beezhold, D. H. (2013). High humidity leads to loss of infectious influenza
virus from simulated coughs. PloS one, 8(2). DOI: 10.1371/journal.pone.0057485
- Van Doremalen, N., Bushmaker, T., Morris, D. H., Holbrook, M. G., Gamble, A., Williamson,
B. N., ... & Lloyd-Smith, J. O. (2020). Aerosol and surface stability of SARS-CoV-2 as compared with
SARS-CoV-1. New England Journal of Medicine. DOI: 10.1056/NEJMc2004973
- Casanova, Lisa M., et al. "Effects of air temperature and relative humidity on coronavirus
survival on surfaces." Appl. Environ. Microbiol. 76.9 (2010): 2712-2717. DOI: 10.1128/AEM.02291-09
- Noti, J. D., Blachere, F. M., McMillen, C. M., Lindsley, W. G., Kashon, M. L., Slaughter,
D. R., & Beezhold, D. H. (2013). High humidity leads to loss of infectious influenza virus from simulated
coughs. PloS one, 8(2). DOI: 10.1371/journal.pone.0057485
- Houtmeyers, E., Gosselink, R., Gayan-Ramirez, G., & Decramer, M. (1999).
Regulation of mucociliary clearance in health and disease. European Respiratory Journal, 13(5),
1177-1188.
- Moriyama, M., Hugentobler, W. J., & Iwasaki, A. (2020). Seasonality of respiratory viral
infections. Annual Review of Virology, 7. DOI: 10.1146/annurev-virology-012420-022445
- Lowen, A. C., Mubareka, S., Steel, J., & Palese, P. (2007). Influenza virus transmission is
dependent on relative humidity and temperature. PLoS Pathog, 3(10),
e151. DOI: 10.1371/journal.ppat.0030151
- Altamimi, A., & Ahmed, A. E. (2019). Climate factors and incidence of Middle
East respiratory syndrome coronavirus. Journal of Infection and Public Health,
In Press. DOI:10.1016/j.jiph.2019.11.011
- Dietz, L., Horve, P.F., Coil, D., Fretz, M., Van Den Wymelenberg, K. (2019).
Novel Coronavirus (COVID-19) Outbreak: A Review of the Current Literature and Built Environment (BE)
Considerations to Reduce Transmission. Preprints 2020, 2020030197.
DOI: 10.20944/preprints202003.0197.v1